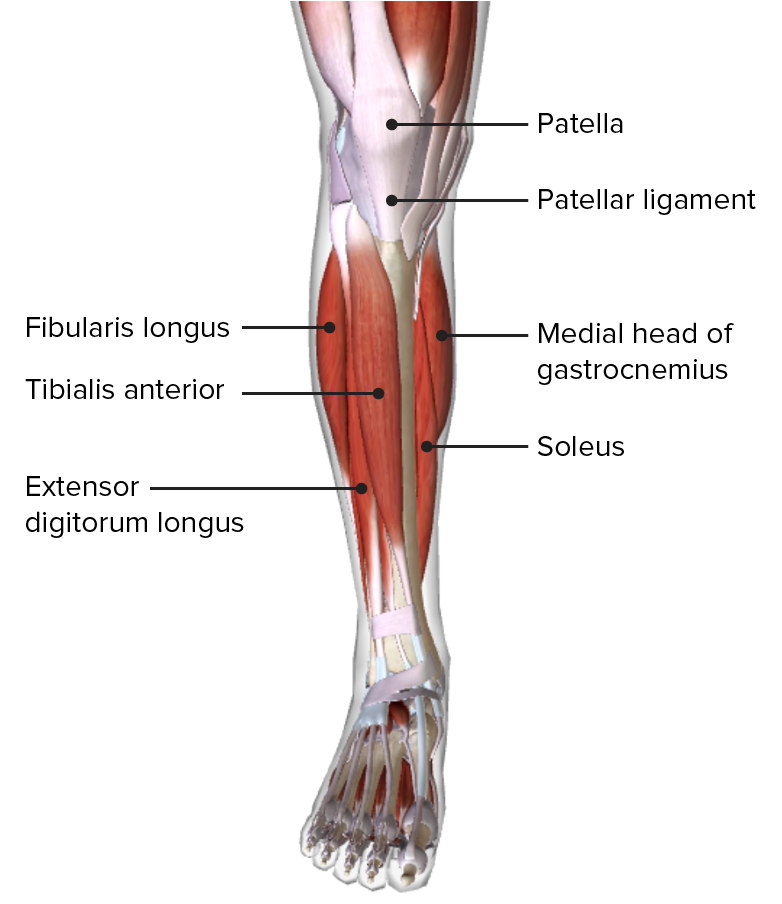
identify interval between superficial & lateral components distally & develop this interval proximally by detaching soleus define the interval between the soleus and the FHL undermine skin posteriorly & perform fasciotomy of superfical posterior compartment perform longitudinal fasciotomy of anterior and lateral compartments undermine skin anteriorly & avoid injuring superficial peroneal nerve proximally identify the common peroneal nerve the incision should be either directly over or slightly posterior to the fibula make incision in line w/ fibula extending just distal to head of fibula to 3 to 4 cm proximal to the lateral malleolus 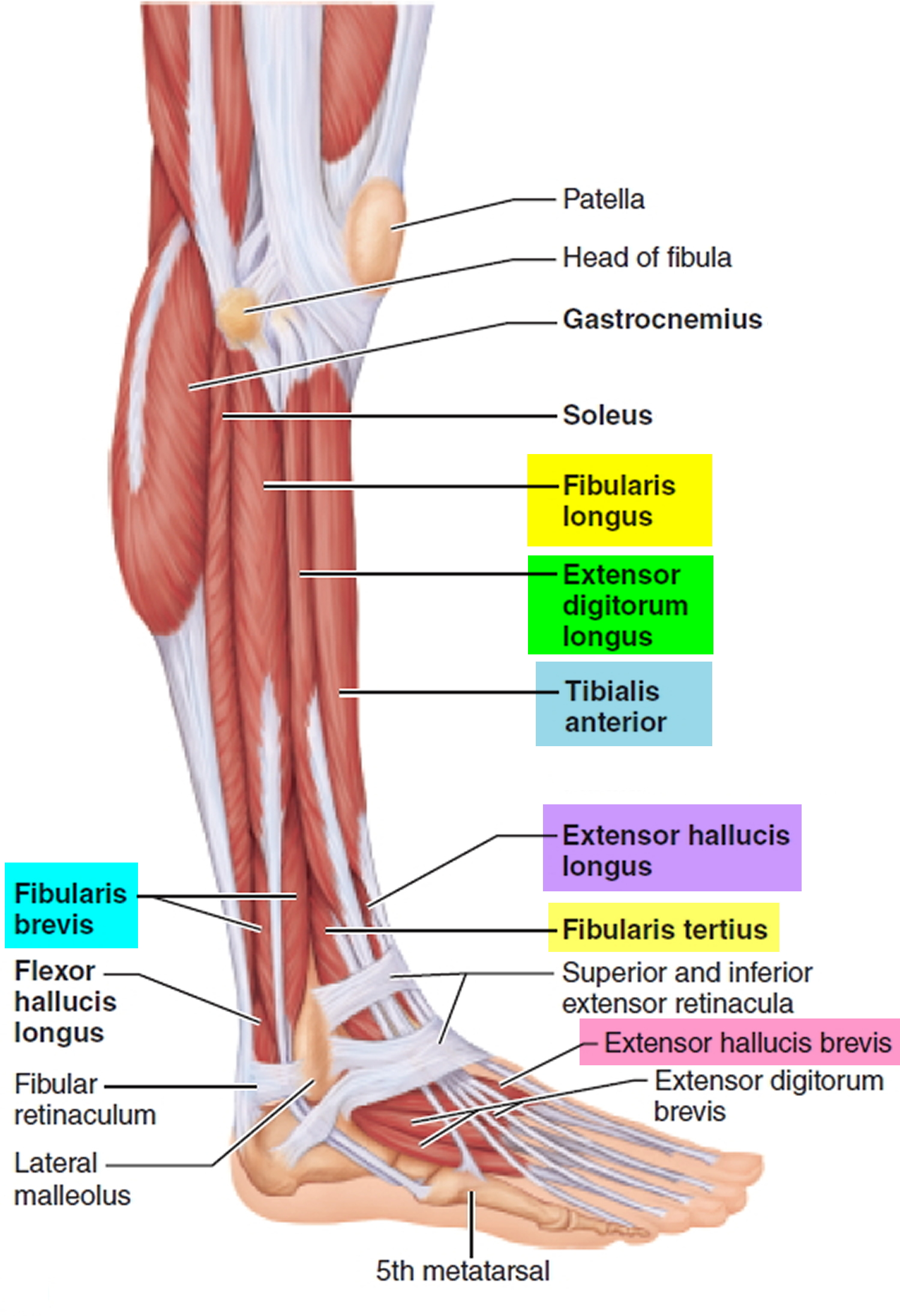
performed thru one long incision over lateral compartment skin grafting is rarely needed if full week is allowed for dissipation of edema wounds are left open if swelling is too much to allow for primary skin closure ref: Compartment Syndrome of the Leg Associated With Frx: An Algorithm to Avoid Releasing the Posterior Compartments. fascia is opened distally and proximally under the belly of soleus again, releasing the fascia over the FDL is required to decompress the deep posterior compartment in the distal half of the tibia the deep posterior compartment lies just below the subcutaneous tissue the neurovascular bundle is protected, lying between the tibialis posterior and the soleus note that the FDL lies just posterior to the tibia, and this fascia needs to be released to decompress the compartment detach soleal bridge and retract it to expose fascia covering FDL & tibialis posterior soleus takes origin from the proximal 1/3 of the tibia and fibula and covers the proximal portion of the deep posterior retract saphenous vein & nerve & release fascia over superfical posterior compartment the saphenous vein should be retracted anteriorly once down to fascia undermine anteriorly to posterior tibial margin, which will avoid saphenous vein and nerve Posterior to posterior medial palpable edge of the tibia deep and superficial posterior compartments are approached thru a single 15 cm longitudinal incision in distal part of leg 2 cm Posteromedial Incision: (Two Incision Technique) once the fascia has been partially transected, tension on the fascia will be lost, which means that the scissors cannot re-enage the if tip of scissors has strayed from fascia, instrument is left in place and two centimeter incision is made over its tip & fasciotomy is superficial peroneal nerve exits from lateral compartment about 10 cm above lateral malleolus and courses into anterior 
distally direct scissors toward lateral malleolus inorder to keep instrument posterior to superficial peroneal nerve distally, avoid straying too medially so as too avoid injury to the dorsalis pedis proximally aim for the patella and distally to the center of the ankle inorder to ensure that the fasciotomy stays in anterior fascia is opened proximally & distally w/ long, blunt-pointed scissors blunt tipped scissors are used to spread above and below the fascia both proximally and distally after identifying septum, small nick is made in fascia of anterior intermuscular septum midway between the septum blunt tipped scissors are used to spread above and below the fascia on both sides of the intermuscular septum, both proximally tension is maintained on the fascia w/ a Kocher clamp attempt to identify the superficial peroneal nerve near the septum transverse incision is made over fascia of anterior & lateral compartments, which allows clear view of the intermuscular septum in the acute traumatic syndrome, a 15 cm incision is used in an elective chronic syndrome, a small 4-5 cm incision can be used incision is therefore placed over anterior intermuscular septum separating anterior & lateral compartments & Shaft, or alternatively placed halfway between the tibial crest and the fibula anterior & lateral compartments are approached thru single longitudinal incision placed halfway down leg 2 cm anterior to fibular Anterolateral Incision: (Two Incision Technique) Compartment Syndromes resulting from Tibial Fractures
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
